Among the different forms of gum disease, gingivitis is the most common to occur in humans, with a prevalence of 59.8% in adults between the ages of 35 and 44, and 51.6% in people between 65 and 74 years. This means that more than half of the population over the age of 35 has gingivitis.
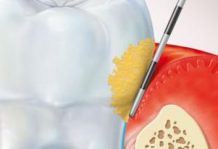
The formation of biofilm on tooth surfaces follows an orderly and dynamic process, which begins with the adhesion of plaque-forming bacteria that accumulate, increasing the mass and complexity of this plaque. If it is not removed, supragingival plaque can reach a level of bacterial complexity so as to cause the onset of gingivitis, which is characterised by several clinical signs: gingival redness, inflammation and bleeding on probing. This is a reversible condition that may lead to periodontitis with a loss of connective tissue attachment.

The microbiota associated with gingivitis is dominated by Actinomyces spp, Capnocytophaga spp. and strict anaerobic gram-negative bacteria. The presence of these bacterial species on gingival tissue causes the formation of a small gingival pocket, or pseudopocket, as a result of junctional epithelium attachment loss or of gingival tissue inflammation.
Bacteria-induced gingival inflammation is the most common form of gingivitis, although gingivitis may also be caused by other factors including trauma, chemical agents, immune defects and ionising radiation, among others.
Gingivitis, being the most prevalent process of all periodontal diseases, is able to develop in people of any age or in any population, although its highest prevalence and severity is detected in adolescence.
 initiative
initiative